What Happens During a Sleep Study in Australia?
Most people are surprised by how routine it feels. The goal is simple: capture a normal night of sleep with enough data for a specialist to interpret.
What is a sleep study, and why would they need one?
A sleep study Australia assessment (often called polysomnography) is an overnight test that tracks sleep and body signals while they rest. They usually need one when symptoms suggest a sleep disorder that cannot be diagnosed reliably from symptoms alone.
Common reasons include loud snoring, witnessed breathing pauses, morning headaches, unrefreshing sleep, and excessive tiredness.
What types of sleep studies are used in Australia?
In Australia, they may be offered an in-lab overnight study or a home sleep test, depending on symptoms and medical history. In-lab studies record more signals and suit complex cases, while home tests often focus on breathing and oxygen for suspected sleep apnoea.
A GP or sleep physician typically decides which option fits their situation.
What happens before the night of the study?
Before the study, they are usually asked about sleep habits, medications, alcohol intake, and typical bedtime routines. They may be given forms or a questionnaire to help the clinic understand their symptoms and risks.
They are often advised to keep their day normal, avoid naps if possible, and follow instructions about caffeine or alcohol.
What should they bring or prepare for a sleep study?
They typically bring comfortable sleepwear, toiletries, and something to read while winding down. If they use regular medications, they usually bring them unless told otherwise.
They should arrive with clean, dry hair and no heavy oils or styling products, since some sensors need good contact.
What happens when they arrive at the sleep clinic?
On arrival, staff confirm details, explain the process, and show them the room. The room often looks like a small hotel room, designed to feel calm and private.
They can usually ask questions, use the bathroom, and get settled before any sensors are attached.
What sensors are attached, and what do they measure?
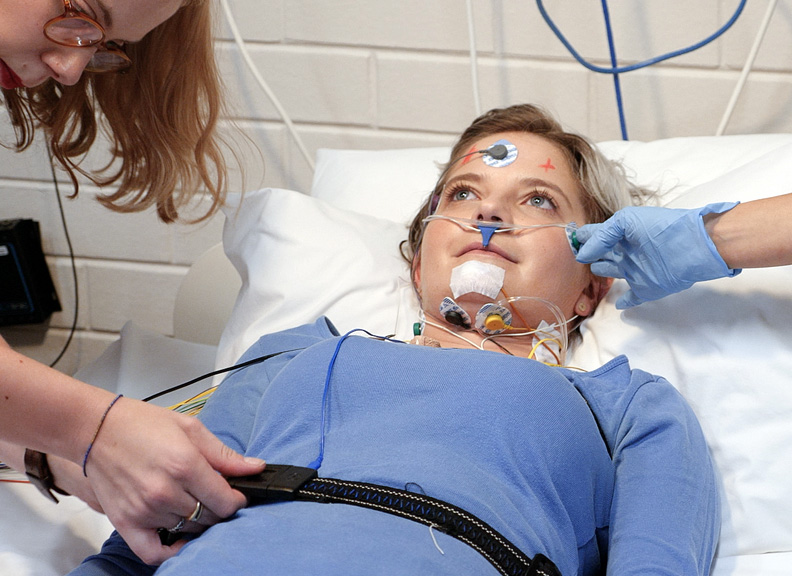
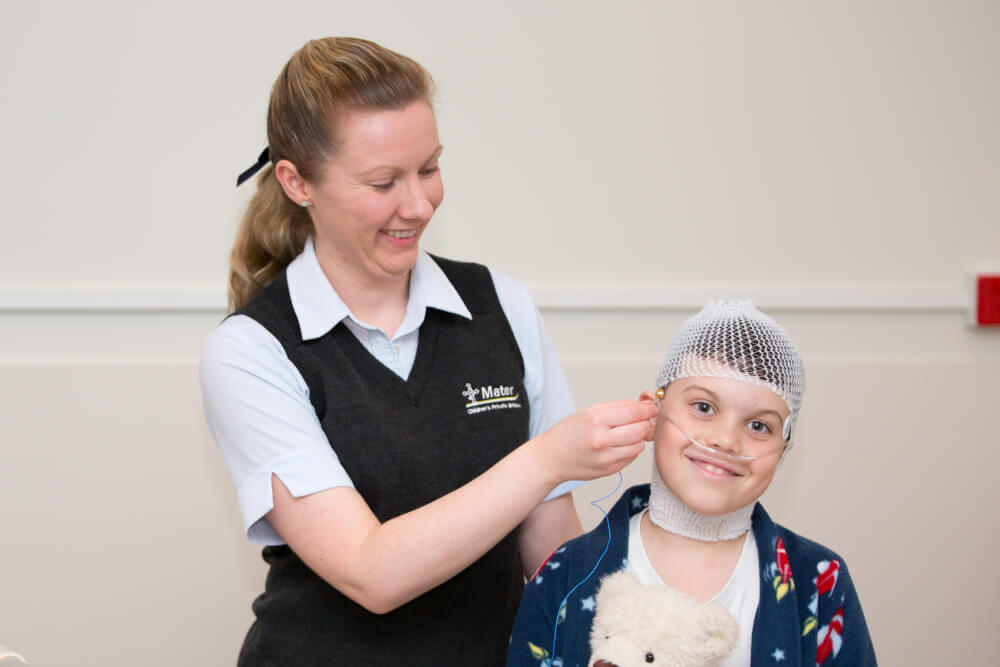
They are fitted with sensors that track sleep stages and body functions throughout the night. These commonly include sticky pads or soft bands placed on the scalp, face, chest, and legs.
Typical measurements include brain activity (sleep stages), eye movement, muscle tone, breathing effort, airflow, snoring, oxygen saturation, heart rate, and limb movements.
Does it hurt, and can they move during the night?
It should not hurt, though it can feel unfamiliar at first. The sensors are designed to stay on while they turn in bed, and the leads are usually gathered to allow reasonable movement.
If something feels too tight or itchy, they can usually call the technician to adjust it.
What is it like trying to sleep during the study?
They are encouraged to sleep as normally as possible, following their usual bedtime. Many people worry they will not sleep, but clinics can still get useful data even if sleep is lighter or shorter than normal.
A camera and audio may be used so the sleep team can match movements or breathing events to the recorded signals. See sleep study cost Australia 2026 pricing and breakdown guide for a detailed overview of current costs and what influences them.
What happens if they need to use a CPAP machine during the study?
If the study strongly suggests sleep apnoea early in the night, they may be offered CPAP partway through to see if it improves breathing and sleep quality. This is sometimes called a split-night study.
If CPAP is introduced, staff typically fit a mask, set pressures, and monitor comfort so they can tolerate it.
What happens in the morning after the study?
In the morning, staff remove the sensors and check whether they have any immediate concerns. They can usually leave shortly after, though they may feel a bit tired if sleep was disrupted.
The data is then analysed and prepared for a formal report, rather than being explained in full on the spot.
How do they get results, and what happens next?
Results are interpreted by a qualified clinician and discussed at a follow-up appointment, often with a sleep physician. They may receive a diagnosis, a severity rating (for sleep apnoea), and a treatment plan.
Next steps might include CPAP, oral appliances, weight or lifestyle strategies, positional therapy, or further testing if symptoms do not match the initial findings.
FAQs (Frequently Asked Questions)
What is a sleep study and why is it important in diagnosing sleep disorders?
A sleep study, or polysomnography, is an overnight test that records breathing, oxygen levels, heart rhythm, and sleep stages to diagnose conditions like obstructive sleep apnoea, restless legs, narcolepsy, or unexplained daytime sleepiness. It provides objective data that cannot be reliably obtained from symptoms alone.
What types of sleep studies are available in Australia and how do they differ?
In Australia, patients may undergo an in-lab overnight sleep study or a home sleep test. In-lab studies record multiple body signals and are suited for complex cases, while home tests primarily monitor breathing and oxygen levels for suspected sleep apnoea. The choice depends on individual symptoms and medical history.
How should I prepare for a sleep study to ensure accurate results?
Before the study, you should maintain your normal daily routine, avoid naps if possible, and follow instructions regarding caffeine or alcohol intake. Bring comfortable sleepwear, toiletries, any regular medications unless advised otherwise, and arrive with clean, dry hair free of heavy oils or styling products to allow proper sensor contact.
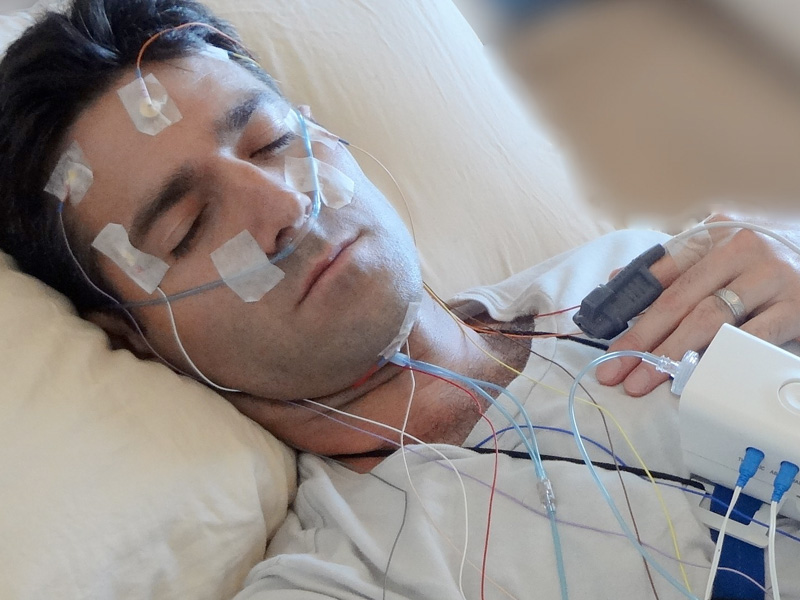
What happens during the night at a sleep clinic and what sensors are used?
Upon arrival at the clinic, staff explain the process and help you settle into a calm, private room. Sensors such as sticky pads or soft bands are attached to your scalp, face, chest, and legs to monitor brain activity (sleep stages), eye movement, muscle tone, breathing effort and airflow, snoring, oxygen saturation, heart rate, and limb movements throughout the night.
Is it uncomfortable to wear sensors during a sleep study and can I move freely?
The sensors used in a sleep study do not hurt but may feel unfamiliar initially. They are designed to stay attached while you turn in bed with leads gathered to allow reasonable movement. If any sensor feels too tight or itchy, you can notify the technician for adjustment.
How will I receive my sleep study results and what treatments might be recommended?
After analysis by a qualified clinician, results are discussed during a follow-up appointment with a sleep physician. You may receive a diagnosis along with severity ratings if applicable. Treatment options could include CPAP therapy, oral appliances, lifestyle changes like weight management or positional therapy, or further testing if needed.
{
"@context": "https://schema.org",
"@type": "BlogPosting",
"mainEntityOfPage": {
"@type": "WebPage",
"@id": "https://villagehealthfoundation.org/sleep-study-australia/"
},
"headline": "What Happens During a Sleep Study in Australia?",
"image": [
"https://villagehealthfoundation.org/wp-content/uploads/2026/03/sleep-study-1000x667-1.jpg",
"https://villagehealthfoundation.org/wp-content/uploads/2026/03/sleep-science-792_x_576.jpg",
"https://villagehealthfoundation.org/wp-content/uploads/2026/03/sleep-study-1.jpg"
],
"author": {
"@type": "",
"name": "Brodie French",
"url": "https://villagehealthfoundation.org/author/admin/"
},
"publisher": {
"@type": "Organization",
"name": "Village Health Foundation",
"logo": {
"@type": "ImageObject",
"url": "https://villagehealthfoundation.org/wp-content/uploads/2022/12/logo-health.png"
}
},
"datePublished": ""
}