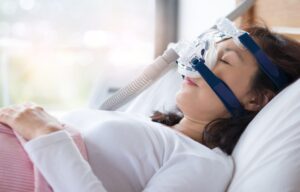
Sleep Apnea and Snoring: Understanding the Overlap
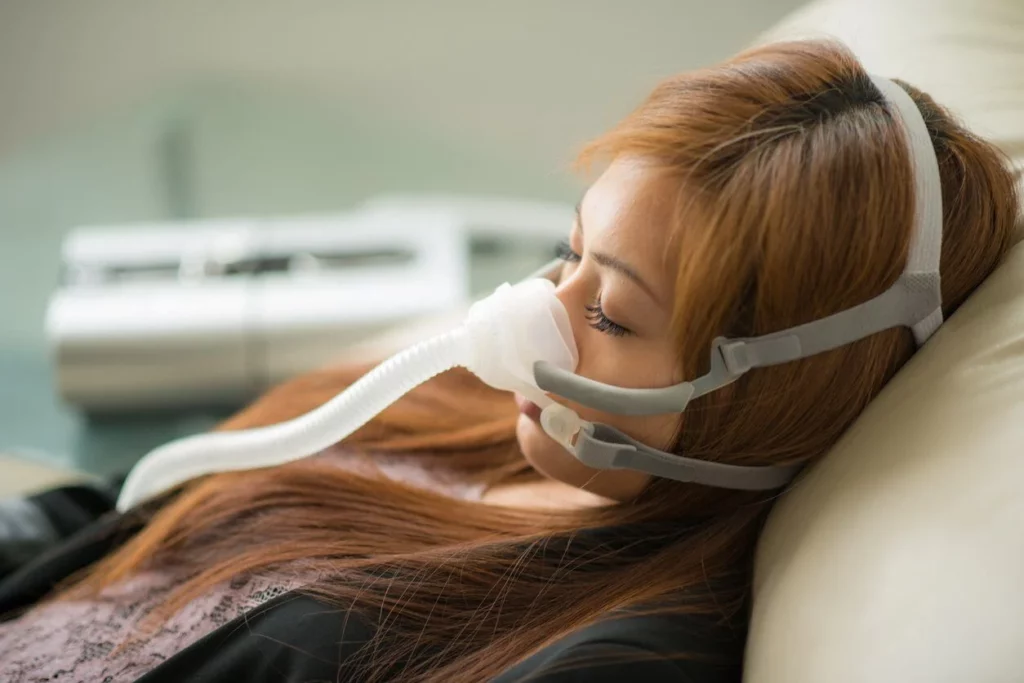
Introduction: When Snoring Is More Than Just Noise
We’ve all heard someone snore — maybe it’s a partner, a family member, or even ourselves. While occasional snoring can be harmless, persistent and loud snoring might be a red flag for something more serious: sleep apnea.
Sleep apnea is a condition where breathing repeatedly stops and starts during sleep. These interruptions prevent restful sleep and reduce oxygen supply to the body, which can put strain on the heart, brain, and other organs. The tricky part? Many people think they just “snore a lot” without realizing they may have a more serious underlying problem.
Understanding the overlap between snoring and sleep apnea can help you recognize the signs, take action early, and protect your long-term health.
Causes of Sleep Apnea: More Than Just a Nighttime Issue
Sleep apnea develops when airflow becomes blocked or disrupted during sleep. This can happen for different reasons, and the causes often overlap with those of habitual snoring.
Obstructive Sleep Apnea (OSA)
This is the most common type and occurs when throat muscles relax too much, causing the airway to narrow or collapse.
See more: How to Travel with a CPAP Machine Without Hassle
Common risk factors include:
- Excess weight – Fat deposits around the neck can narrow the airway.
- Anatomy – A naturally narrow airway, enlarged tonsils, or certain jaw shapes can increase risk.
- Age – Risk rises after age 40, though it can occur at any age.
- Gender – Men are more likely to develop OSA, though post-menopausal women also face higher risk.
- Family history – Genetics can play a role in airway structure.
Central Sleep Apnea (CSA)
Less common, CSA happens when the brain fails to send proper signals to breathing muscles. It’s often linked to conditions like heart failure or neurological disease.
Lifestyle Triggers
Certain daily habits and conditions can worsen both snoring and sleep apnea:
- Alcohol before bed (relaxes throat muscles too much)
- Sedative medications
- Smoking (inflammation and fluid retention in airway)
- Chronic nasal congestion
- Sleeping on the back (gravity makes airway collapse more likely)
Example:
David, 46, believed his loud snoring was just “part of getting older.” But after his wife noticed pauses in his breathing at night, a sleep study revealed moderate OSA. His risk factors — recent weight gain, nightly wine, and a habit of sleeping on his back — were all contributing to the problem.
Symptoms: The Obvious and the Overlooked
While loud snoring is one of the most common symptoms of sleep apnea, it’s far from the only one. Some warning signs are easy to spot, while others are subtle enough to be missed for years
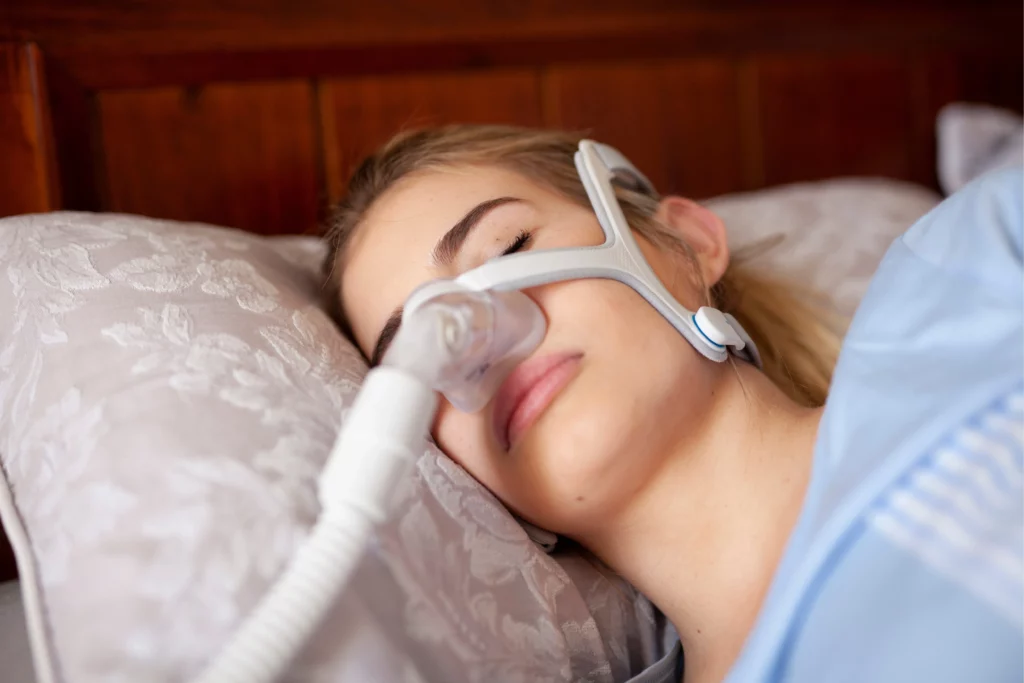
Common Symptoms
- Loud, chronic snoring (often disruptive to others)
- Breathing pauses observed during sleep
- Waking up gasping or choking
- Excessive daytime sleepiness
- Morning headaches
Subtle or Overlooked Symptoms
- Difficulty concentrating during the day
- Mood changes, irritability, or depression
- Waking up with a dry mouth or sore throat
- Forgetfulness and slower reaction times
- Falling asleep easily during quiet moments (reading, watching TV, or sitting in traffic)
Example:
Maria, 52, didn’t think she had sleep apnea because she wasn’t “that tired” during the day. But she often woke with headaches and had trouble focusing at work. After her daughter mentioned hearing her snore and gasp for air while napping on the couch, Maria got tested — and discovered she had severe OSA.
Why Snoring and Sleep Apnea Overlap
Not all snoring means sleep apnea, but most people with sleep apnea snore. Snoring occurs when airflow causes the tissues in the throat to vibrate. In sleep apnea, these tissues can collapse entirely, stopping airflow altogether.
Think of it like a garden hose: snoring is when water still flows but makes a rattling noise; sleep apnea is when the hose is kinked and water stops flowing completely. Both involve airway narrowing — but sleep apnea adds a dangerous pause in breathing.
Treatment Options: Restoring Peaceful Sleep
Fortunately, sleep apnea can be treated effectively once diagnosed. The right approach depends on the severity of the condition, the underlying cause, and the patient’s preferences.
1. CPAP Therapy
Continuous Positive Airway Pressure (CPAP) is the most common and effective treatment for moderate to severe OSA. It delivers steady air pressure through a mask, keeping the airway open all night.
Benefits:
- Highly effective when used consistently
- Improves daytime energy and cognitive function
- Reduces risk of heart-related complications
Challenges:
- Some find the mask uncomfortable at first
- Requires regular cleaning and maintenance
2. Oral Appliances
These dentist-fitted devices adjust the jaw or tongue position to keep the airway open. They’re especially useful for mild to moderate OSA or for people who can’t tolerate CPAP.
3. Surgery
For certain structural problems, surgical options may help — such as removing excess throat tissue, repositioning the jaw, or correcting nasal blockages. Surgery is generally considered when other treatments fail.
4. Lifestyle Changes
Lifestyle adjustments can greatly improve symptoms, especially for mild cases:
- Weight loss – Even small reductions can ease airway pressure.
- Positional therapy – Using pillows or special devices to avoid back-sleeping.
- Avoiding alcohol and sedatives before bedtime.
- Quitting smoking to reduce airway inflammation.
5. Treating Nasal Congestion
Addressing allergies or chronic sinus problems can improve airflow and reduce both snoring and apnea episodes.
Example:
Tom, 38, had mild OSA and didn’t want to use a CPAP. His doctor recommended an oral appliance, weight loss, and side-sleeping. Within four months, his snoring dropped significantly, and his energy levels returned.
The Importance of Diagnosis
Because snoring and sleep apnea share symptoms, it’s easy to dismiss warning signs as “just noise.” But ignoring potential sleep apnea is risky. Untreated, it can lead to:
- High blood pressure
- Heart disease and stroke
- Type 2 diabetes
- Depression and anxiety
- Increased accident risk due to daytime fatigue
A sleep study — whether done in a lab or at home — is the only way to confirm a diagnosis and guide proper treatment.
Conclusion: Don’t Ignore the Signs
If you or someone you love snores regularly — especially if it’s paired with pauses in breathing, morning headaches, or daytime fatigue — it’s worth getting checked for sleep apnea.
Sleep isn’t just about rest; it’s about giving your body the oxygen and recovery time it needs to stay healthy. Treating sleep apnea not only quiets the snoring but can transform your energy, focus, and overall well-being.
The overlap between snoring and sleep apnea means that what sounds like a minor annoyance could actually be an early warning sign. Paying attention now can protect your health for years to come.
If you want, I can also create a short patient